If your prostate exam or the result of your PSA test indicates the possibility of cancer, your doctor may order diagnostic imaging tests. These are more complex types of prostate exams that allow urologists to “see” the gland, either through ultrasound, radio waves, or x-rays. None of these prostate exams can diagnose cancer 100 percent: a biopsy is necessary to make the final diagnosis.
Trans Rectal Ultrasound (TRUS)
A trans rectal ultrasound uses high frequency sound waves to generate an image of the prostate. A probe is lubricated, and inserted into the rectum. The probe then emits sound waves that are reflected back to the probe by the prostate and other organs. The returned ultrasound waves are used to construct a picture of the gland.
Computed Tomography (CT Scan)
Computed tomography, also known as a CT scan, uses x-rays to generate computerized cross sections of the internal organs. Multiple x-rays are taken during a CT scan, providing the urologist with an overall view of the gland.
Magnetic Resonance Imaging (MRI)
Unlike computed tomography, which uses potentially harmful x-rays, magnetic resonance imaging (MRI) uses magnets and radio waves to generate a 3-dimensional image of internal organs. The resolution of the MRI is so detailed that urologists can tell the difference between cancerous and healthy tissue, even if those changes are very slight.
Proton Magnetic Resonance Spectroscopic Imagery (MRSI)
An MRSI is performed in combination with an MRI. Like magnetic resonance imaging, an MRSI uses magnetic and radio waves. An MRSI, however, can detect differences at the cellular level. A MRSI can detect levels of certain cellular chemicals (metabolites) that will be in low concentrations if prostate cancer is present.
ProstaScint Scan
The ProstaScintTM scan uses injected radioisotopes to locate cancer. The isotopes are injected into the bloodstream, and attach themselves to cancerous cells. Accumulations of the radioisotopes can then be found using a special gamma ray camera. The test is not 100 percent accurate; false positive results have been made.
Radionuclide Bone Scan
Your urologist may suggest a bone scan, to determine whether the cancer has spread to the bones or not. In early-stage prostate cancer, this is usually a precautionary test, performed to rule out possible complications.
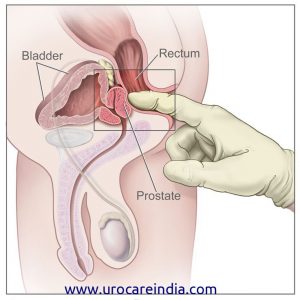
Prostate Cancer Screening
Screening for prostate cancer is a controversial topic. The concern is not that digital rectal exams and prostate specific antigen (PSA) results cannot identify early-stage cancers. Both sides agree that this is true. Opponents of regular screening suggest that positive screening results may lead to unnecessary prostate cancer treatment and needless anxiety.
PSA Results and The Case For Screening
PSA results and other forms of screening allow men to access prostate cancer treatment during the early stages of their disease. Whether immediate treatment is required or not, symptoms can be monitored in case the condition worsens. Early screening and early detection, proponents argue, can save lives. The argument is simple, but powerful.
The Case Against Screening
The argument against screening is somewhat more complex. A recent study by the U.S. Preventive Services Force states that no hard evidence indicates that early detection of prostate cancer affects the eventual outcome of the disease. Most men diagnosed with prostate cancer are over the age of 65. Only three percent of men diagnosed will die from the disease. As the disease progresses very slowly, in most cases, most men diagnosed will actually die from other causes.
While fifteen percent of American males will be diagnosed with the disease, only eight percent actually need surgery or other treatment. Early detection, opponents argue, often leads to unnecessary treatment. Surgery and radiation therapy can have unwanted side effects, including urinary incontinence, bowel dysfunction and erectile dysfunction.
Opponents object to the needless anxiety and stress that a diagnosis generates. If early detection of the disease will not change the outcome, they argue, why bother upsetting men with the test results? Perhaps this is a case where what men don’t know won’t hurt them.
Watchful Waiting
For many men, a diagnosis of prostate cancer results in what urologists refer to as “watchful waiting.” Symptoms of the disease are monitored, but treatment is not undertaken unless symptoms increase in severity.

The Choice is Yours
Choosing whether to undergo prostate testing or not is an individual decision. Some men prefer to know; some would just as happily remain unaware. The same reasoning applies to treatment side effects: some men would prefer to have early treatment, and run the risk of side effects. Others would prefer to wait and see if their symptoms worsen. Of course, your decision should be based on relevant issues such as age and risk factors, like a family history of prostate disease.
The information on this site explores the different types of prostate cancer screening.
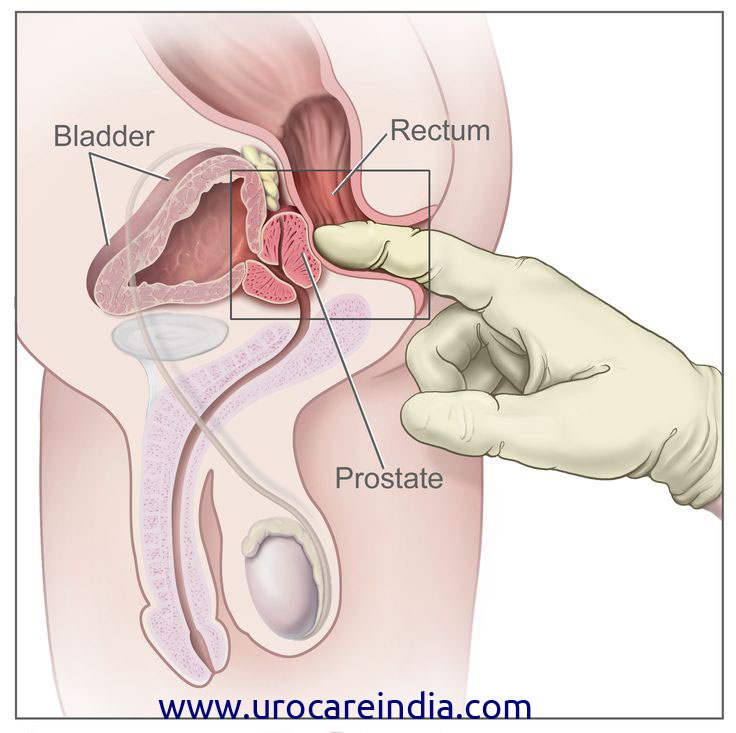
The American Cancer Society recommends that men over the age of 50 should get digital rectal exams (DREs) on a regular basis.
The prostate specific antigen (PSA) test is a blood test that is used frequently to screen for prostate cancer.
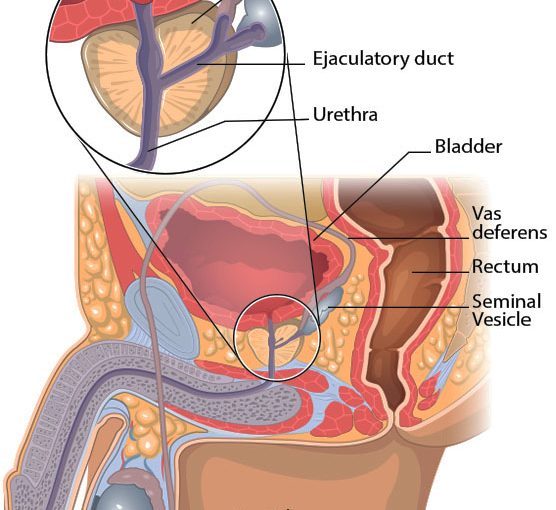
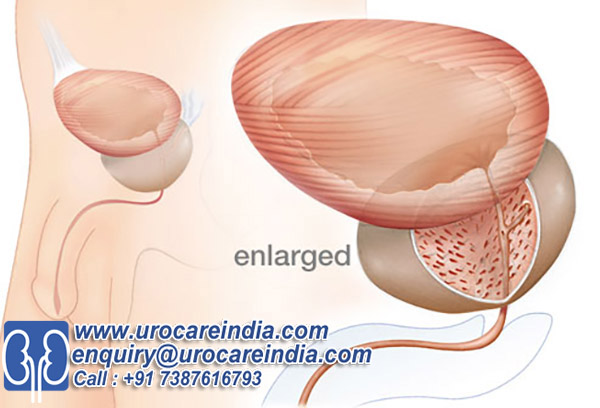
Often called the visual prostate exam, prostate imaging will allow urologists to actually see the prostate gland.
Though screening can give urologists some information, the only real way to confirm that a man has prostate cancer is to conduct a tissue biopsy of the area.
RESOURCE: http://www.urocareindia.com/